MercoPress. South Atlantic News Agency
World Health Organization calls for urgent action to curb hepatitis
 WHO is alerting people to the risks of contracting hepatitis from unsafe blood, unsafe injections, and sharing drug-injection equipment.
WHO is alerting people to the risks of contracting hepatitis from unsafe blood, unsafe injections, and sharing drug-injection equipment. 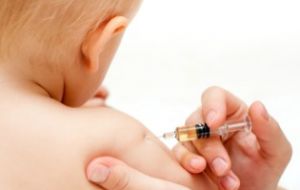 WHO recommends vaccinating all children against hepatitis B infection, from which approximately 780 000 people die each year.
WHO recommends vaccinating all children against hepatitis B infection, from which approximately 780 000 people die each year.  This year WHO’s flagship event takes place in Egypt, estimated to have 10% of the population between 15 and 59, chronically infected with hepatitis C.
This year WHO’s flagship event takes place in Egypt, estimated to have 10% of the population between 15 and 59, chronically infected with hepatitis C. On World Hepatitis Day (28 July) the World Health Organization highlights the urgent need for countries to enhance action to prevent viral hepatitis infection and to ensure that people who have been infected are diagnosed and offered treatment. This year, the Organization is focusing particularly on hepatitis B and C, which together cause approximately 80% of all liver cancer deaths and kill close to 1.4 million people every year.
WHO is alerting people to the risks of contracting hepatitis from unsafe blood, unsafe injections, and sharing drug-injection equipment. Some 11 million people who inject drugs have hepatitis B or C infection. Children born to mothers with hepatitis B or C and sex partners of people with hepatitis are also at risk of becoming infected.
The Organization emphasizes the need for all health services to reduce risks by using only sterile equipment for injections and other medical procedures, to test all donated blood and blood components for hepatitis B and C (as well as HIV and syphilis) and to promote the use of the hepatitis B vaccine. Safer sex practices, including minimizing the number of partners and using barrier protective measures (condoms), also protect against transmission.
Approximately, two million people a year contract hepatitis from unsafe injections. These infections can be averted through the use of sterile syringes that are specifically designed to prevent reuse.
Eliminating unnecessary injections is also an effective strategy to protect against hepatitis transmission. There are 16 billion injections administered every year. Around 5% of these injections are for immunization, a further 5% for procedures like blood transfusions and injectable contraceptives, and the remaining 90% to administer medicines. For many diseases, injections are not the first recommended course of treatment and oral medications could be used.
WHO recommends vaccinating all children against hepatitis B infection, from which approximately 780 000 people die each year. A safe and effective vaccine can protect from hepatitis B infection for life. Ideally, the vaccine should be given as soon as possible after birth, preferably within 24 hours. The birth dose should be followed by 2 or 3 doses to complete the vaccine series.
WHO also recommends vaccinating adults who are at increased risk of acquiring hepatitis B. These include people who frequently require blood or blood products (for example dialysis patients), health-care workers, people who inject drugs, household and sexual contacts of people with chronic hepatitis B, and people with multiple sexual partners.
Since 1982, over 1 billion doses of hepatitis B vaccine have been used worldwide and millions of future deaths from liver cancer and cirrhosis have been prevented. In a number of countries where around 1 in 10 children used to become chronically infected with the hepatitis B virus, vaccination has reduced the rate of chronic infection to less than 1 in 100 among immunized children. To date, there is no available vaccine against hepatitis C.
Medicines are now available that can cure most people with hepatitis C and control hepatitis B infection. People who receive these medicines are much less likely to die from liver cancer and cirrhosis and much less likely to transmit the virus to others. WHO therefore urges people who think they might have been exposed to hepatitis to get tested so they can find out whether they need treatment to improve their own health and reduce the risk of transmission.
Earlier this year, WHO issued new guidelines for treatment of hepatitis B infection. These recommend using simple non-invasive tests to assess the stage of liver disease to help identify who needs treatment. WHO also calls for prioritizing treatment for those with cirrhosis - the most advanced stage of liver disease and for the use of two safe and highly effective medicines, tenofovir or entecavir. Continued monitoring using simple tests is important to assess whether treatment is working, and if it can be stopped.
In 2014, WHO issued guidance for testing and treatment of hepatitis C infection. WHO recommends providing testing for people considered at high risk of infection and ensuring treatment for those who have the virus with several effective medicines, including new regimens that use only oral medicines. WHO will update recommendations on drug treatments periodically as new antiviral medicines become available and as new evidence emerges.
This year, WHO’s flagship event takes place in Egypt, a country that has one of the world’s highest hepatitis burdens. It is estimated that 10% of the population between 15 and 59 years is chronically infected with hepatitis C. Between 2007 and 2014, more than 350 000 people with hepatitis C have been treated. Since the introduction of newer, more effective medicines in 2014, the number of people being treated continues to increase. Today, 32 dedicated treatment centres are providing treatment at the Government’s expense.
Egypt is also highlighting hepatitis prevention. WHO is helping the country develop national blood safety standards and has selected it as one of 3 pilot countries for its new Global Injection Safety Initiative. WHO will provide support over the next 3 years to reduce unnecessary injections and help transition to the exclusive use of syringes that can only be used once.
In September this year, countries will have the opportunity to share best practice at the first-ever World Hepatitis Summit to be held in Glasgow, Scotland. The summit, which is co-sponsored by WHO, the Scottish Government and the World Hepatitis Alliance, aims to raise the global profile of viral hepatitis, to create a platform for exchange of country experiences and to focus on working with countries to develop national action plans.



Top Comments
Disclaimer & comment rulesCommenting for this story is now closed.
If you have a Facebook account, become a fan and comment on our Facebook Page!